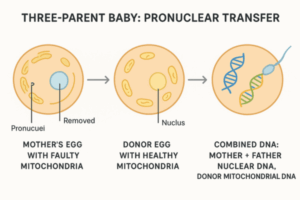
Oocyte Donation Donor Screening Process: In 2026, fertility programs reported that about 71% of people who first inquire about becoming oocyte donors withdraw before finishing screening, which shows just how selective and involved the donor screening process really is.
Key Takeaways
| Question | Answer |
|---|---|
| What is the oocyte donation donor screening process? | It is a stepwise evaluation of potential egg donors, including eligibility checks, medical history, lab testing, and counselling, before they can donate eggs in programs like Oocyte Donation at The Life Fertility Clinic. |
| Who decides if a donor is eligible? | Clinicians at specialist centers, such as those described in the Fertility Clinic Guide, assess whether a donor meets age, health, and risk criteria. |
| What age are oocyte donors usually? | Current guidance in 2026, such as ASRM recommendations, commonly focuses on donors in their early twenties to mid-thirties, and surveys show that 94.6% of donors are under 35. |
| Is genetic testing part of donor screening? | Most programs include some form of genetic evaluation, and an international survey reported that 83.3% of oocyte-donor centers perform genetic testing, alongside embryo-focused options like Preimplantation Genetic Testing (PGT). |
| How does oocyte donation fit into assisted reproductive technology? | Oocyte donation sits within a wider suite of ART options explained in the Assisted Reproductive Technology overview, alongside IVF, ICSI, and IUI. |
| What treatments may use donor oocytes? | Donor eggs can be fertilised in IVF procedures, sometimes with techniques like ICSI, and embryos are then transferred to the recipient. |
| Where can recipients learn more or ask questions? | Recipients can contact specialist teams directly through pages like Contact Us at The Life Fertility Clinic to discuss donor programs. |
1. Why Donor Screening Matters In Oocyte Donation Programs
Oocyte donation depends on a careful screening process that protects donors, recipients, and future children as far as current evidence and regulations allow.
In 2026, programs treat donor screening as a structured pathway from first inquiry to active donor status, and only a minority of potential donors complete it.
We approach screening as a way to gather accurate information, offer clear counselling, and ensure that everyone involved can give informed consent.
It is not possible to guarantee specific medical outcomes, and we always encourage patients and donors to discuss individual risks and benefits with qualified fertility specialists.
2. Step 1: Initial Inquiry And Pre‑screening For Egg Donors
The donor screening journey usually starts with an online or phone inquiry and a structured questionnaire.
At this stage, many potential donors realise the commitment involved and decide that donation is not right for them, which contributes to the 71% withdrawal rate reported in research.

Pre-screening questions often cover age, BMI range, smoking or vaping status, major medical conditions, and family health history.
We use this early information to decide whether a potential donor should proceed to a more detailed assessment or whether another pathway might be more suitable.
3. Step 2: Age, Medical, And Lifestyle Eligibility For Oocyte Donors
In 2026, professional guidelines such as ASRM recommendations commonly suggest that oocyte donors fall within a specific age window, often 21 to 34 years old.
Programs may still consider donors outside this range, but they typically disclose donor age to recipients and may request additional psychological evaluation for younger donors.
Medical eligibility typically considers chronic illnesses, reproductive history, medications, and infection risk factors.
Lifestyle criteria can include nicotine use, recreational drugs, heavy alcohol intake, or high risk sexual behaviour, which clinics explore in donor interviews.
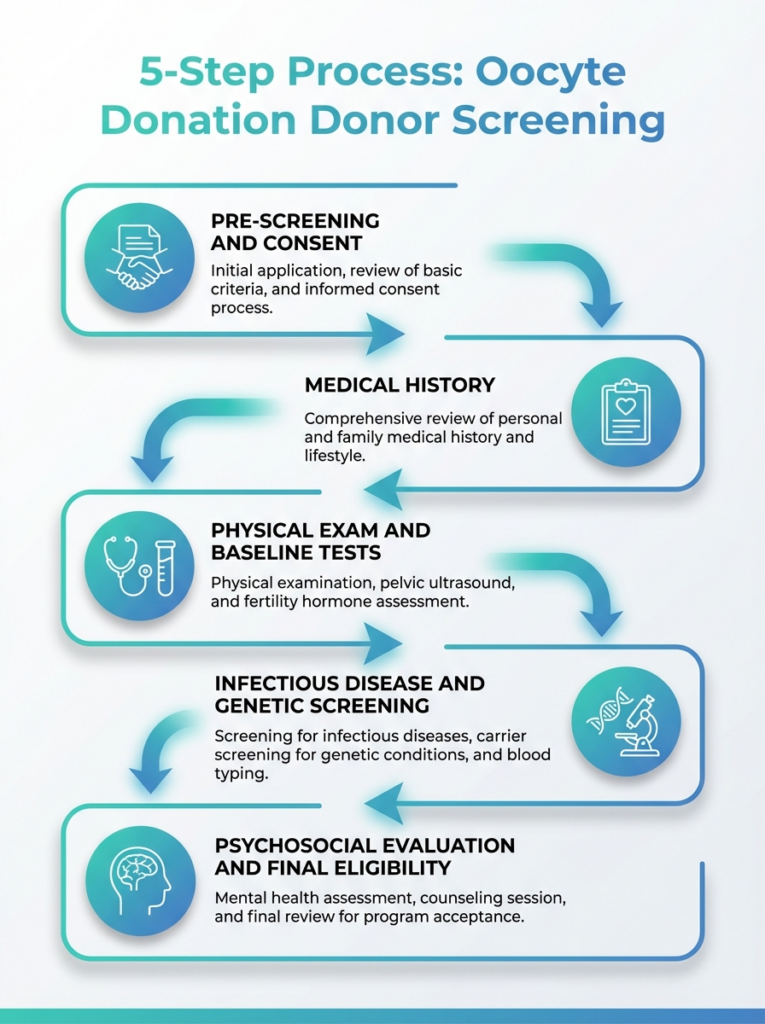
This infographic outlines the five-step screening process for oocyte donors. It highlights eligibility checks, testing, consent, and ethical considerations.
4. Step 3: Clinical Examination And Laboratory Testing
Once a donor passes initial eligibility checks, we arrange a physical examination and a tailored panel of laboratory tests.
These usually include screening for certain infections, baseline hormone levels, and a detailed pelvic or ultrasound assessment, although exact tests vary by clinic and jurisdiction.
Many centers also include carrier screening for inherited conditions, because an international survey found that 83.3% of oocyte donor centers perform genetic testing on donors.
We always explain what each test can and cannot detect so that donors and recipients have realistic expectations about screening limits.
Did You Know?
12% of people who make an initial inquiry about becoming an oocyte donor eventually enter the active donor pool after screening.
5. Step 4: Psychological Assessment And Counselling For Donors
Oocyte donation is not only a medical process, it is also a long term personal decision, so psychological assessment is a core part of screening.
In 2026, many guidelines advise that donors, especially younger ones, meet with counsellors experienced in reproductive ethics and third party reproduction.
These sessions help donors explore how they feel about anonymity, future contact, disclosure to their own partners or children, and the possibility of future genetic matching technologies.
Counsellors also check that donors understand the treatment schedule, the time commitment, and the limits of what screening can anticipate.
6. Step 5: Legal Consent, Anonymity, And Donor Limits
Before a donor can proceed to a stimulation cycle, we complete detailed consent documents that set out rights, responsibilities, and privacy arrangements.Globally, around 91.3% of donors have historically been anonymous or nondirected, although open identity and known donor arrangements are now more common in some regions.
Professional bodies also suggest limits on how many donation cycles a single donor undertakes; for example, ASRM guidance in 2026 refers to a maximum of six oocyte donation treatment cycles per donor.
These limits are designed to manage donor safety and to reduce the chance that many genetic half-siblings will be conceived in a small geographic area.
7. How Donor Screening Connects To IVF, ICSI, And ART Treatment Pathways
Once an oocyte donor is accepted, her eggs are usually involved in IVF-based treatments for recipients, and sometimes ICSI is used to inject a single sperm into each egg.
The quality and completeness of donor screening can influence how clinics plan treatment strategies, monitoring schedules, and additional embryo testing options.
Research from 2013 to 2020 shows that donor oocyte embryo transfer cycles accounted for around 12.4% of all ART transfer cycles at one point, decreasing to approximately 8.8% by 2020.
These shifting patterns influence how clinics staff donor programs, schedule stimulation cycles, and allocate laboratory resources for frozen and fresh donor material.
Did You Know?
The total cost to bring a single donor into an oocyte donation program, including screening and evaluation, was estimated at approximately $1,869 in published analyses.
8. Costs, Timeframes, And Program Capacity In 2026
Screening a donor involves staff time, counselling, labs, and administration, which is why published estimates place the cost of bringing one screened donor into a program at around $1,869.
Because most inquiries do not reach active donor status, clinics spread these costs across their entire donor pool when planning budgets and recipient pricing.
From a timing perspective, the full donor screening process can take several weeks or longer, depending on how quickly appointments and test results are completed.
We always advise both donors and recipients to discuss expected timelines at the outset, since these influence when a stimulation cycle can realistically start.
9. Recipient Experience: What Our Patients Need To Know About Donor Screening
For recipients, understanding the donor screening process can bring reassurance that a structured system is in place, but it is also important to recognise what screening does not guarantee.
No screening protocol can rule out every possible health issue, and we are careful not to make promises about future outcomes or the health of any resulting child.
We encourage recipients to ask detailed questions about how donors are recruited, which tests are performed, and how information is shared.
A transparent conversation with the clinic team can help recipients weigh oocyte donation against other pathways such as donor embryo adoption or further autologous IVF attempts.
10. Future Trends: Data, Genetics, And Ethical Questions In 2026
By 2026, oocyte donation programs will increasingly work with frozen eggs and embryos, and earlier data show that the proportion of frozen donor embryo transfers among all donor oocyte cycles rose from about 42.3% in 2013 to 76.6% in 2020.
This shift puts more focus on laboratory quality systems, cryopreservation protocols, and robust documentation of donor screening results that follow each batch of eggs or embryos.
At the same time, genetic matching technologies and direct-to-consumer DNA testing raise fresh questions about anonymity and future contact between donors and donor-conceived adults.
We expect donor screening conversations in 2026 and beyond to include realistic discussion of these possibilities so that donors and recipients can make choices that fit their values.
Conclusion
The oocyte donation donor screening process in 2026 is a multi step pathway that combines eligibility checks, clinical testing, psychological evaluation, and legal consent.
Only a small proportion of initial inquiries become active donors, which reflects how carefully programs evaluate each person before their eggs are used in treatments such as IVF and ICSI.
As a fertility team, we aim to use the best available evidence, clear communication, and thoughtful counselling at each step, while avoiding unsupported medical claims or unrealistic promises.
If you are considering becoming a donor or using donated oocytes, we recommend arranging a detailed consultation with a specialist clinic so you can discuss the screening process in the context of your own situation and questions.