Oocyte Donation Success Rates are a key consideration when exploring fertility options. Oocyte donation can offer a strong path to pregnancy when using your own eggs is not possible, but success depends on more than just the donor eggs themselves. In 2026, patients are asking sharper questions about real-world outcomes, risks, and what factors actually move the needle.
Key Takeaways
| Question | Short Answer |
|---|---|
| 1. What is oocyte donation and how does it relate to success rates? | Oocyte donation uses eggs from a screened donor that are fertilized in the lab and transferred to the recipient’s uterus. Success rates depend on donor egg quality, sperm quality, embryo development, and uterine health, which we explain in detail on our oocyte donation guide. |
| 2. Who typically benefits most from donor eggs? | Patients with low ovarian reserve, repeated IVF failures with their own eggs, or certain genetic concerns may consider donor eggs, as outlined on our dedicated egg donation information page. |
| 3. Which medical procedures influence donor-egg IVF outcomes? | IVF protocols, lab techniques, and add-ons like ICSI and PGT can influence the overall pathway. You can see how these fit together on our IVF procedures and treatments overview. |
| 4. How can genetics affect donor egg success? | Embryos created from donor eggs may be checked for certain genetic or chromosomal issues using PGT, which can help clinics select embryos with a higher likelihood of resulting in a healthy ongoing pregnancy. Learn more on our Preimplantation Genetic Testing (PGT) page. |
| 5. What role does sperm quality play in donor egg cycles? | Sperm quality can affect fertilization and embryo development, so techniques like ICSI are sometimes used. We outline when this may be considered on our ICSI information page. |
| 6. Are donor embryos an alternative if donor egg cycles are not suitable? | Some patients consider donor embryo adoption, which uses embryos donated by another couple. The framework is described on our donor embryo adoption page. |
| 7. Where can I read about real experiences with fertility treatments? | Patient stories can help set realistic expectations, which is why we share them on our testimonials page. |
Understanding Oocyte Donation and Why Success Rates Matter
Oocyte donation is a form of assisted reproductive technology in which a healthy donor provides eggs that are fertilized in a laboratory, then transferred to a recipient’s uterus. In 2026, more individuals and couples are looking at donor eggs not just as a last resort, but as a considered option when time, age, or medical conditions affect their own egg quality.
Success rates provide a rough guide to what might be possible, but they never guarantee a result for any one person. Our role is to help you understand the moving parts so you can ask clear questions and partner with your clinic in a realistic way.
How Clinics Typically Describe Oocyte Donation Success Rates
Clinics in 2026 usually talk about donor egg success in terms of probabilities, not promises. Common measures include per-cycle clinical pregnancy rate, ongoing pregnancy rate, and live birth rate, which can all differ.
Public clinic statistics must be interpreted with care, because they are averages that blend many different ages, diagnoses, and treatment plans. Your own probability depends on your medical history, uterus and endometrium, sperm parameters, and the way your clinic manages the cycle.
| Measure | What it describes |
|---|---|
| Fertilization rate | How many donor eggs successfully fertilize in the lab, often influenced by sperm quality and lab technique. |
| Blastocyst formation rate | How many embryos reach day 5 to 6, which is one indicator of embryo development potential. |
| Per-transfer clinical pregnancy rate | Percentage of embryo transfers with a heartbeat seen on ultrasound. |
| Live birth rate per transfer | Percentage of transfers that result in a live birth. |
We do not publish specific numerical rates on these pages because outcomes vary across patients and protocols. Instead, we focus on explaining the factors you can discuss with your care team when you consider oocyte donation.
Key Biological Factors That Influence Donor Egg IVF Outcomes
Biology still sits at the center of any oocyte donation cycle. While donor eggs typically come from younger, screened donors, egg quality can still vary between individuals.
In 2026, clinics pay particular attention to four biological pillars: donor egg quality, sperm quality, embryo development, and uterine receptivity. No single factor guarantees a result, but problems in any of these areas can lower overall chances.
- Donor egg quality can shape fertilization and embryo development.
- Sperm quality affects how many eggs fertilize and how embryos grow.
- Embryo quality is often graded visually, sometimes alongside PGT data.
- Uterine receptivity depends on lining thickness, timing, and hormonal preparation.
Important: Two patients can use donor eggs through the same clinic and still see very different outcomes. This is why clinics emphasize individualized assessment instead of generic promises.
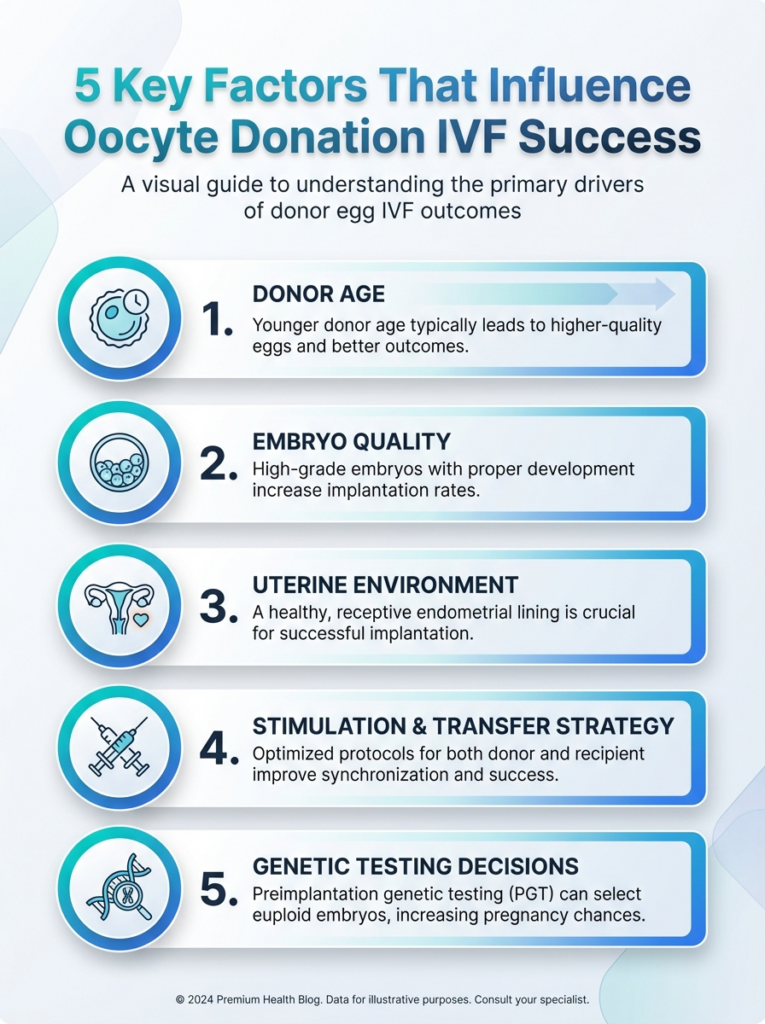
This infographic highlights the five key factors that influence oocyte donation IVF success and how they affect outcomes. Use it to contextualize success rates when discussing options with a clinic.
Age, Diagnosis, and When Egg Donation Is Usually Considered
In 2026, many patients reach fertility clinics later in life, often after trying naturally or through multiple IVF cycles with their own eggs. Age can affect egg quantity and quality, so donor eggs may be discussed when repeated cycles show poor response or when ovarian reserve testing suggests limited potential.
Egg donation may also be considered when there is a risk of passing on serious genetic conditions or when previous treatments have led to recurrent poor embryo quality. Our oocyte donation guides explain these scenarios so you can prepare for a detailed conversation with a specialist.
- Diminished ovarian reserve or early menopause.
- Repeated IVF failure with own eggs.
- Certain inherited genetic conditions.
- Previous cancer treatments that affected ovarian function.
Every situation is different, so the decision to move to donor eggs is typically made after reviewing investigations, age, and previous treatment history, as well as your emotional readiness.
The IVF Lab, ICSI, and Their Role in Donor Egg Cycles
Once donor eggs are collected, the lab becomes central to your chances of success. The IVF team prepares sperm, inseminates or injects eggs, and monitors embryo growth day by day.
Intracytoplasmic sperm injection, or ICSI, places a single sperm directly into each egg. In 2026, clinics may use ICSI when there is male factor infertility, previous poor fertilization, or certain lab indications.
| Approach | What happens | Potential influence on outcomes |
|---|---|---|
| Conventional IVF | Many sperm are placed with each egg and fertilization occurs in the dish. | Can work well when sperm parameters are normal. |
| ICSI | A single sperm is injected into each egg using a fine needle. | Can improve fertilization in certain sperm issues, but does not guarantee embryo quality. |
It is important to understand that ICSI and other lab techniques are tools, not guarantees. Your clinic will usually explain why a particular approach fits your situation and how it relates to your broader donor egg plan.
Preimplantation Genetic Testing (PGT) and Embryo Selection
Some donor egg cycles in 2026 include preimplantation genetic testing, or PGT, to assess embryos before transfer. PGT can look for certain inherited single-gene conditions (PGT-M) or structural chromosomal rearrangements (PGT-SR), depending on your circumstances.
Because PGT involves embryo biopsy and detailed genetic analysis, clinics use it selectively rather than automatically for every donor egg cycle. The goal is to help reduce the risk of passing on specific known conditions or structural chromosomal problems.
- PGT does not create healthy embryos, it helps identify embryos with particular genetic patterns.
- Not all patients need or benefit from PGT, especially where risk of genetic disease is low.
- Any decision to use PGT should be made with thorough counseling about pros and limitations.
When you look at success statistics that mention PGT, remember that those figures often reflect a pre-selected group of patients with specific indications, not the general donor egg population.

Endometrial Preparation, Transfer Strategy, and Cycle Planning
Even with strong donor eggs and good embryos, the uterus must be prepared carefully for transfer. In 2026, clinics use hormonal preparation or natural-cycle approaches to align the embryo transfer with the most receptive window of the endometrium.
Factors that can influence your individual probability of success include endometrial thickness, timing of progesterone exposure, and the presence or absence of uterine issues like polyps or large fibroids. Ultrasounds and sometimes additional procedures aim to address these before transfer.
- Fresh vs frozen transfer: Some programs use frozen embryo transfers to allow more controlled timing.
- Single vs double embryo transfer: Transferring more than one embryo can increase the chance of twins and related risks.
- Cryopreservation: Extra embryos may be frozen for later use if the first transfer does not lead to a pregnancy.
Careful planning can increase the chance that each embryo transfer is given the best opportunity in your individual circumstances, but there is always an element of biological uncertainty.
Donor Egg vs Donor Embryo: Comparing Pathways and Outcomes
While oocyte donation uses donor eggs and usually the recipient’s or partner’s sperm, donor embryo adoption involves embryos that another couple has created and donated. In 2026, some patients explore both, especially when they want a simpler path that does not require separate donor and sperm choices.
These options differ in genetics, legal framework, and emotional experience, which can matter as much as the raw probability of pregnancy. Donor embryo adoption may involve fewer decisions during the cycle, but less genetic connection for one or both intended parents.
| Aspect | Oocyte Donation | Donor Embryo Adoption |
|---|---|---|
| Genetic link | Recipient or partner may share genetics via sperm. | No genetic link to either intended parent. |
| Decision-making | Choose donor plus sperm source. | Choose existing embryos created by another couple. |
| Embryo creation | Embryos created fresh for you or with donor eggs. | Embryos are already created and frozen. |
Success probabilities for each path are influenced by similar biological factors, such as embryo quality and uterine health, but you should also weigh legal, ethical, and personal preferences as part of your decision.
Emotional, Physical, and Financial Factors Behind the Numbers
Numbers alone do not capture what it feels like to pursue oocyte donation. Patients in 2026 consistently tell us that the decision involves grief about using their own eggs, hope for a future child, and practical concerns about time, cost, and work or family commitments.
Your tolerance for multiple cycles, your support network, and your financial resources all influence what a realistic plan looks like. Even when a clinic’s per-cycle pregnancy rate appears high, some people will still need more than one attempt or may decide to stop before pregnancy occurs.
- Emotional load: Counseling can help manage expectations and family discussions.
- Physical demands: Medication schedules, monitoring visits, and possible procedures.
- Financial planning: Budgeting for donor fees, cycle costs, potential PGT, and embryo storage.
These elements do not directly change the biology of a single embryo transfer, but they do shape whether you feel able to continue if the first attempt does not succeed.
How To Interpret Success Statistics Carefully in 2026
When you compare success rates between clinics or programs, it is easy to feel pulled toward the highest number on the page. In reality, several hidden variables can make side by side comparisons misleading.
For example, some clinics treat a higher proportion of older or complex patients, some transfer more than one embryo per cycle, and some include or exclude certain groups from their published figures. Asking how data is collected and which patients are included can give you a more realistic picture.
- Ask whether the rates are per cycle started, per transfer, or per patient.
- Check if the statistics separate donor eggs from own-egg IVF.
- Find out how often single embryo transfer is used.
- Clarify which age groups and diagnoses the data represents.
Ultimately, the most useful number is the one that applies to patients similar to you, using a pathway similar to the one your team recommends, rather than a headline rate that mixes many different situations.
Conclusion
Oocyte donation in 2026 offers a meaningful route to pregnancy for many people whose own eggs are unlikely to lead to a successful outcome, but it is not a guarantee for anyone. Success rates depend on a network of factors, including donor egg quality, sperm parameters, embryo development, uterine preparation, and the specific strategies your clinic uses.
The most useful step you can take is to bring informed questions to your consultation, asking not only about headline numbers, but about how those figures relate to your age, diagnosis, and treatment plan. With realistic expectations and clear communication, you can decide whether oocyte donation fits your goals, your values, and the path you feel ready to take.