Preimplantation Genetic Testing (PGT) is increasingly becoming part of fertility care in Nigeria and across Africa. In 2025, the Nigerian market for preimplantation genetic diagnosis—a form of PGT—was projected at around USD 1.42 million, reflecting growing interest among couples seeking genetic insights into their embryos before IVF transfer. While still less common than in high-resource countries,
PGT is now offered in several Nigerian fertility clinics, particularly for couples at risk of inherited conditions or those experiencing repeated IVF challenges. Understanding what happens to embryos during PGT can help prospective parents make informed decisions and navigate assisted reproductive technology with greater confidence.
Key Takeaways
| Question | Short Answer |
|---|---|
| What is preimplantation genetic testing (PGT)? | PGT is a laboratory method used with IVF to study the genetic makeup of embryos before transfer, which we describe in detail on our Preimplantation Genetic Testing (PGT) page. |
| Who usually considers PGT? | Couples with known inherited conditions, recurrent pregnancy loss, repeated IVF failures, or advanced maternal age often discuss PGT as part of their IVF procedures and treatments planning. |
| Is PGT the same as IVF? | No, PGT is an add‑on test used with IVF, which is one category of assisted reproductive technology (ART) that involves fertilizing eggs outside the body. |
| Can donor eggs or embryos be tested? | In many clinics, embryos created with donor eggs or donor embryos can also be considered for PGT as part of oocyte donation or donor embryo adoption pathways, depending on the program protocols. |
| Does PGT guarantee a healthy baby? | No, PGT does not guarantee outcomes, it focuses on specific genetic findings and still has limitations, which we explain in our assisted reproductive technology articles. |
| Where can I read more about fertility topics related to PGT? | You can browse our broader education hub on fertility and IVF in the fertility and IVF categories, which we keep updated in 2026. |
| How do I talk to someone about PGT? | You can reach us directly via our contact page to ask questions or schedule a consultation. |
1. What Preimplantation Genetic Testing (PGT) Really Is In 2026
When we talk about preimplantation genetic testing in 2026, we are describing a laboratory method that studies embryos created through IVF before any transfer to the uterus happens. Our goal is to help you understand what the test can and cannot tell you so that you can make informed choices with your specialist.
PGT happens in the context of assisted reproductive technology; it is not something that can be done in a natural cycle without IVF. We position PGT as one possible step on your journey, not as a promise or guarantee of a particular outcome.
Types of PGT You Will Hear About
Clinics commonly describe three broad categories: PGT for single‑gene conditions (often called PGT‑M), PGT for structural rearrangements (PGT‑SR), and PGT for chromosome number (often discussed as PGT‑A). Each category targets a different type of genetic question.
For example, PGT‑M may be considered when a couple carries a well‑defined single‑gene condition, while PGT‑SR is more focused on chromosome rearrangements such as translocations. PGT‑A, which looks at chromosome counts, is widely discussed, but its use remains an individual decision that should be made with detailed counseling.
2. Step 1: Consultation And Fertility Workup Before PGT
Every PGT journey in 2026 still begins with a careful consultation, not with a lab test. During your first visit, we review your history, previous pregnancies or losses, and any known family conditions that might influence whether PGT is relevant.
We also discuss other assisted reproductive options, such as IUI or conventional IVF, so you have context before you commit to a more complex path. This helps you understand how PGT fits within the broader set of fertility treatments.
Testing And Planning Before IVF With PGT
Before any eggs are collected, we usually suggest a combination of fertility tests such as ovarian reserve assessments, sperm analysis and ultrasound, which we detail in our broader IVF procedure guides. The purpose is to design an IVF plan that aligns with your health, your timeline and your preferences.
Once this assessment is complete, your specialist can outline whether PGT is being considered for a specific genetic reason or more general embryo assessment, and they can describe the step‑by‑step lab pathway you can expect.
3. Step 2: IVF Cycle, Egg Collection, And Fertilization
Because PGT studies embryos in the laboratory, it is always paired with IVF. First, your ovaries are stimulated with medications so that multiple mature eggs can be collected in a single procedure.
On the day of egg collection, a sperm sample is prepared in the lab, then eggs and sperm are combined through conventional IVF or intracytoplasmic sperm injection (ICSI), depending on your specific plan.
Why ICSI Is Often Used With PGT
ICSI is a specialized IVF method where a single sperm is injected into each mature egg using a fine needle under the microscope. Many centers prefer ICSI for embryos that will undergo PGT because it reduces the chance that extra sperm DNA on the outside of the egg might complicate test interpretation.
ICSI is not mandatory in all PGT cases, but in 2026, it remains a common combination, particularly where there are male factor considerations or where the clinic protocol favours ICSI for tested embryos.
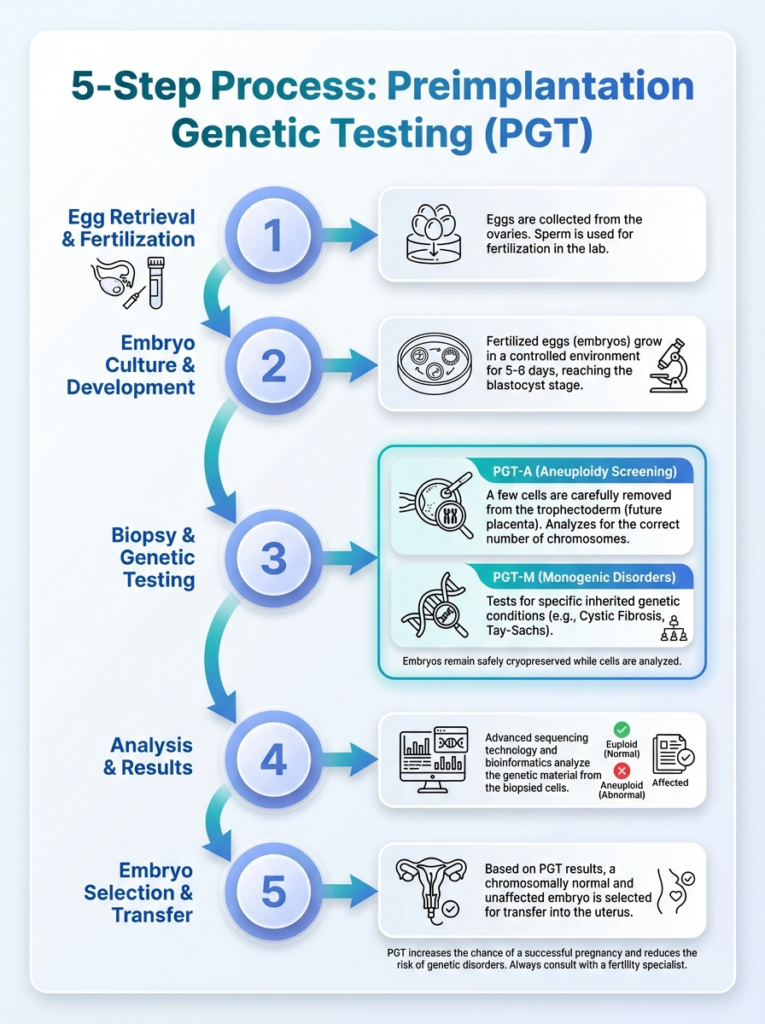
This infographic breaks down the 5-step Preimplantation Genetic Testing (PGT) process. It highlights key steps and outcomes for prospective parents.
4. Step 3: Embryo Development And Timing Of The Biopsy
After fertilization, the embryos are cultured in the lab for several days while embryologists monitor their development. Around day 5 or 6, many PGT programs perform biopsies at the blastocyst stage, which is when the embryo has formed a fluid-filled cavity and distinct cell groups.
In this stage, cells that will later form the placenta are usually the ones sampled, while the inner cell mass that would become the baby is left intact. This approach aims to collect genetic material without removing cells directly from the inner cell mass.
How Embryo Biopsy Works In Practice
During a biopsy, a tiny opening is made in the outer layer, and a small number of cells are gently removed and placed in a separate tube for analysis. The embryo itself is then usually frozen while the genetic test is being performed.
Some published data show that biopsy results can be obtained for a high percentage of embryos, one committee report noted results in 97.2% of cleavage stage embryos in earlier protocols, although methods and outcomes can differ between clinics and over time.

Did You Know?
Post-visit patient knowledge scores were 80.8% with a handout plus brief genetic counseling versus 46.9% with provider-only counseling, highlighting how structured education can improve understanding of PGT decisions.
5. Step 4: Genetic Analysis Of The Biopsied Cells
Once the biopsy samples leave the embryology lab, they enter a separate genetic testing workflow. Different methods may be used depending on whether your clinic is assessing single genes, chromosome rearrangements, or whole chromosome copy numbers.
What all methods have in common is that they study DNA from the sampled cells to look for specific changes that the team has agreed to test for in advance. The scope of what is tested is not unlimited; it reflects the panel or assay chosen for your case.
How To Interpret PGT Results Carefully
Results often use categories such as “no reportable abnormality detected for the tested condition,” “affected for the tested condition,” “carrier,” or “inconclusive,” especially with PGT‑M and PGT‑SR. For PGT‑A, reports frequently classify embryos as euploid, aneuploid, or sometimes mosaic, depending on the lab protocols.
In some expert reviews of PGT‑A, a high proportion of embryos from certain groups have been reported as aneuploid, for example one source mentioned 78.6% aneuploid embryos in a specific cohort, which illustrates how complex human embryo genetics can be rather than predicting any individual couple’s numbers.

6. Step 5: Embryo Freezing, Selection, And Transfer Planning
While the genetic analysis is underway, your embryos are usually kept safe through cryopreservation, which means controlled freezing and storage. This allows time for the test to be completed without pressuring you to transfer before the report is available.
Once the results return, your specialist will sit with you to review each embryo and discuss which ones, if any, are suitable for transfer based on the testing scope and your goals. This is where clear communication and realistic expectations are essential.
Thawing And Frozen Embryo Transfer
When you are ready for transfer, one or sometimes more embryos are thawed and prepared for placement into the uterus, usually in a separate frozen embryo transfer cycle. The timing of this cycle is coordinated with your natural or medicated endometrial preparation.
In 2026, many clinics favour single embryo transfer policies in most PGT cycles to limit the risks associated with multiple pregnancies, although specific decisions are always individualized and should be discussed in detail.
7. Who Typically Considers PGT In 2026
PGT is not offered to every IVF patient in the same way, and not everyone needs it. In many programs, PGT‑M and PGT‑SR are mainly discussed with couples who have identified single gene conditions or chromosomal rearrangements in their personal or family history.
PGT‑A is more often brought up with people who have had repeated IVF failures, recurrent pregnancy losses, or those in advanced maternal age brackets, although practice patterns vary between countries and clinics.
PGT With Donor Eggs Or Donor Embryos
Some patients explore PGT in the context of egg donation or embryo adoption, especially if they want as much information as possible about donor‑conceived embryos. Oocyte donation can be relevant when ovarian reserve is low or when genetic issues are present in the intended mother.
Donor embryo adoption can also intersect with PGT discussions, although programs differ in whether testing has already been done on stored embryos or whether additional testing is feasible or allowed.
Did You Know?
Two weeks after education, patient knowledge about PGT was reported as 79.6% with a handout plus brief counseling versus 49.9% with provider-only counseling, showing how follow-up materials can help people remember complex information.
8. Benefits, Limits, And Ethical Questions Around PGT
People are often interested in PGT because it can provide additional information about embryos before transfer, particularly when specific genetic conditions are a concern. This information can support decision-making about which embryos to transfer and in what order.
However, PGT has limits, and it does not test for every possible condition or guarantee future health. Some embryos yield inconclusive results, and in some contexts, test findings can be complex to interpret, especially with mosaic or borderline classifications.
Considering Published Data Carefully
Some expert opinions have associated PGT‑A in specific groups with outcomes such as lower miscarriage rates per transfer or shorter time to a pregnancy resulting in live birth, but those findings are based on particular study designs and patient populations. Clinical benefit can differ between individuals, and there are ongoing debates and studies in this field in 2026.
Because we do not want to overstate what any single study can show, we always recommend using published data as part of a balanced conversation with your fertility specialist rather than as a promise of what your own cycle will deliver.
9. How PGT Fits Alongside Other Fertility Treatments
PGT sits within a whole spectrum of assisted reproductive technologies, rather than existing in isolation. For some couples, less invasive options such as intrauterine insemination (IUI) may be appropriate before considering IVF with PGT.
IUI involves placing prepared sperm directly into the uterus around the time of ovulation and does not involve embryo creation in the lab, so PGT is not part of that procedure.
ART Options And Long‑Term Planning
For others, combining IVF, PGT, and cryopreservation can support long‑term family planning, especially if you wish to preserve embryos for future transfers. Fertility preservation pathways may be considered for medical or personal reasons before genetic testing is even on your radar.
In 2026, we encourage people to see PGT as one component in a broader strategy that might include lifestyle changes, timed intercourse or IUI, IVF, egg or sperm donation, or embryo adoption, depending on your medical picture and your values.
10. Questions To Ask Your Clinic Before You Start PGT
Because PGT is detailed and highly technical, we suggest going into your consultation with a written question list. This can help you feel more prepared and make the most of your appointment time.
Effective communication has been shown in studies to improve understanding of PGT significantly, especially when written materials are used in addition to verbal explanations, which is one reason we invest in clear guides like this in 2026.
Checklist Of Practical Questions
- Why are you recommending PGT in our specific case, and which type are you suggesting?
- Exactly what will the test look for, and what will it not look for?
- How will biopsy be performed in your lab, and how will embryos be handled and stored?
- How long do results usually take, and how will they be explained to us?
- What are the possible result categories, and how might they influence our embryo transfer decisions?
- What other options would we have if we choose not to proceed with PGT?
Writing the answers down or asking for a summary can also support partners who are not able to attend every visit, and can help you revisit the information calmly at home.

Conclusion
Preimplantation genetic testing in 2026 is a multi step journey that runs from consultation and IVF planning through to embryo biopsy, genetic analysis, freezing, and carefully timed transfer. At every stage, our focus is on clear information and realistic expectations rather than guarantees.
If you are considering PGT, taking the time to understand each step can help you feel more confident and calmer as you move forward. We are here to walk you through the details, answer questions, and help you decide whether this pathway fits your medical picture and personal values.